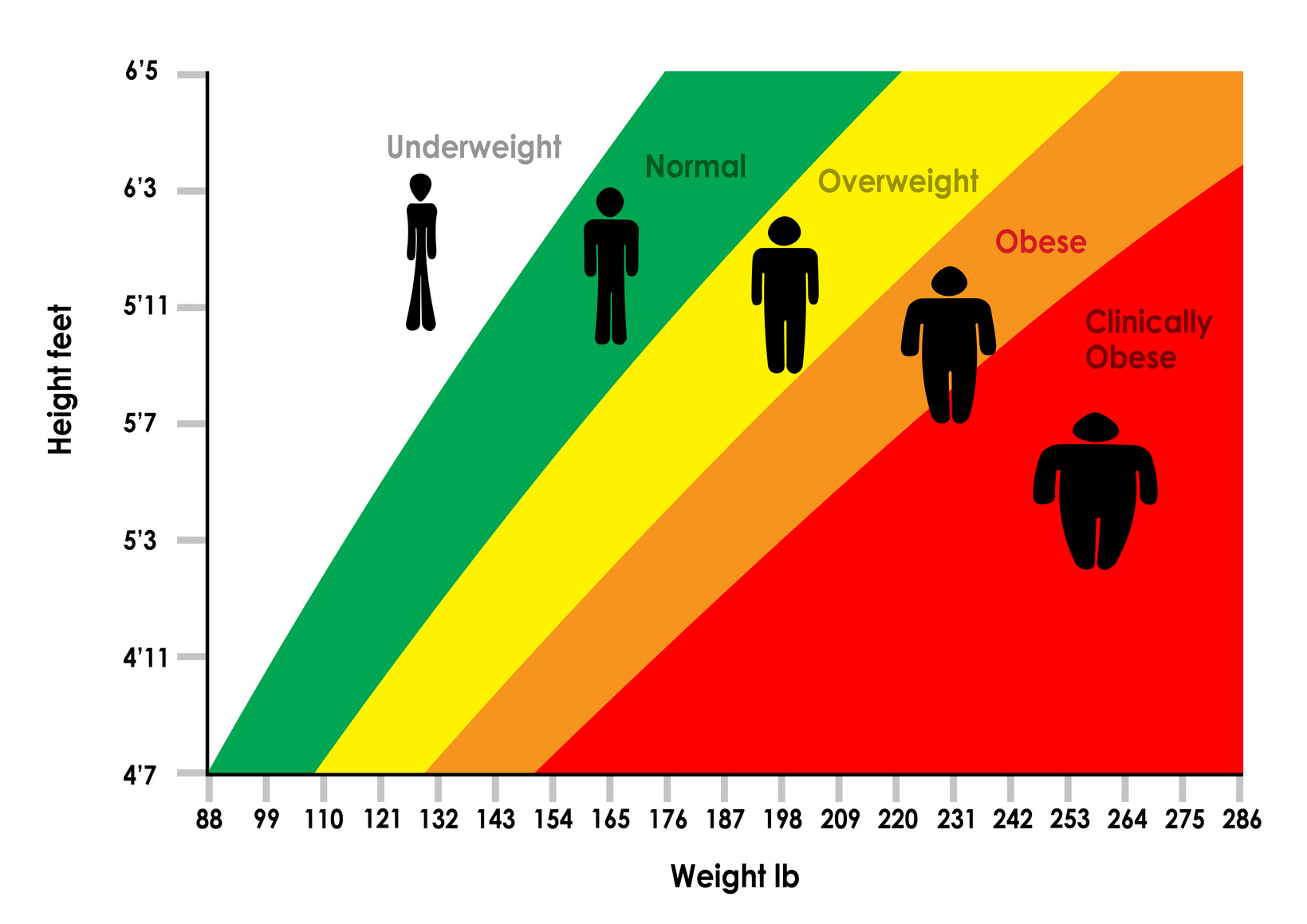
The proportion of internal fat increases and muscle mass decreases with age, which can lead to sarcopenic obesity, the combination of obesity and muscle impairment 22. Women have a significantly higher percentage of total and sub-cutaneous fat stores than their male counterparts 21. For example, South Asian populations have a higher proportion of body fat than Caucasians for the same BMI 20. The proportion of body fat also differs across ethnic populations, sex, and age groups. 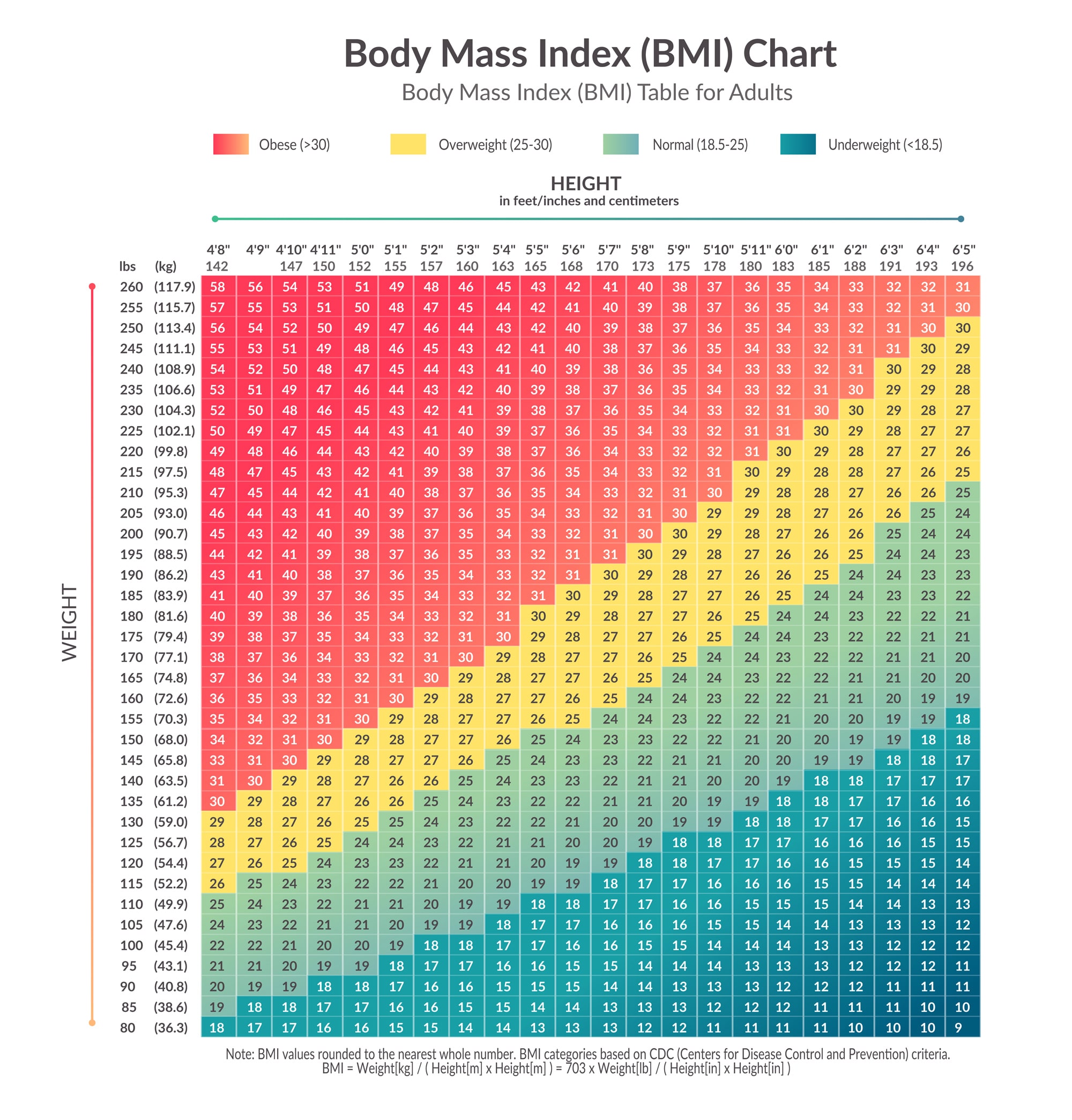
Not all people with high levels of body fat have a BMI of 30 or greater, and some people with very high BMIs may have little fat mass. Indeed, one of the main deficiencies of BMI is that it does not differentiate between fat mass and fat-free mass. In older age, overweight and obesity as defined by BMI might even be protective against mortality 17, 18, 19. Although a significantly higher mortality rate was found for all obesity grades combined (hazard ratio 1.18 ), being overweight (BMI of 25–< 30) reduced the risk of all-cause mortality (0.94 ), and grade 1 obesity (BMI of 30–< 35) was not related with higher mortality (0.95 ) 16. For mortality, this association follows a J-shaped curve. 
They have called for a new definition that fully accounts for the complexity of the disease relating to the quantity, distribution and secretory function of adipose tissue.Ī substantial body of evidence has shown that obesity (BMI ≥ 30) is associated with an increased risk of coronary heart disease 15 and mortality 16 relative to normal weight. However, several researchers and professional associations 8, 9, 10, 11, 12, 13, 14 consider the use of BMI as the primary clinical index of obesity insufficient. Adults with a BMI greater than or equal to 30 are classified as being obese 1 (Table 1). It is most commonly assessed using body mass index (BMI), a simple and quick anthropometric tool that has a low cost. WHO conceptualises obesity as “abnormal or excessive fat accumulation that may impair health” 1. Because it can be difficult for physicians to accurately determine obesity solely through visually inspecting their patients 7, they need a reliable, efficient screening tool in order to ensure that those who need management and treatment receive it. Individual studies indicate that patients are more likely to lose weight when they receive recommendations for lifestyle changes from their primary care physicians 6. Primary care is considered one of the main settings for the prevention, screening and management of obesity 5. Associations have been shown to be strongest between obesity and the incidence of diabetes mellitus, particularly in women (risk ratio 12.41, 95% confidence interval 9.03–17.06). Obesity increases the risk for many chronic diseases, such as diabetes mellitus, cardiovascular diseases and cancers 3, and is possibly associated with mental health disorders 4. These numbers have almost tripled since 1975 2. According to the World Health Organization (WHO), in 2016 more than 650 million adults worldwide were obese 1. Obesity is widely recognised as a pandemic public health problem. However, due to the lack of more accurate and feasible alternatives, BMI and WC might still have a role as initial tools for assessing individuals for excess adiposity until new evidence emerges. No evidence supports that WHR and WHtR are more suitable than BMI or WC to assess body fat. In conclusion, BMI and WC have serious limitations for use as obesity screening tools in clinical practice despite their widespread use. The data were insufficient to pool the results for waist-to-hip ratio (WHR) and waist-to-height ratio (WHtR) but were similar to BMI and WC. The aim of this systematic review was to assess the performance of anthropometric tools to determine obesity in the general population (CRD42018086888).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
